In keeping with the Socialist principle that the State must own and control everything, as with the ANC’s National Health Insurance Scheme, the National Treasury said it was also moving forward with the establishment of a state-owned bank for South Africa, and that Cyril Ramaphosa, and the Minister of Finance, Tito Mboweni, were supporting it. It might surprise many to discover that the Central Bank is in fact privately owned, as it is worldwide.
Continue reading…
ANC Government wants to Establish a State Bank, in Line with their Socialist Principles. Hint: Central Banks are Private!
Enjoyed this post? Share it!
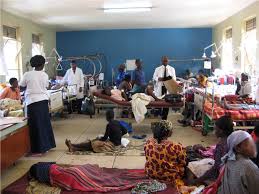
How Covid19 Kills Innocent People Who DON’T Have Covid19! Kidney Patient Neglected & Left to Die in Tshepong State Hospital!
Collateral Damage: Did Covid restrictions let a man literally starve to a lonely death, in yet another horror story from a state hospital, preventing his family from noticing and helping him? Allowed to die from hunger and dehydration in Tsheponh hospital in Klerksdorp? By now everyone should be aware of what death traps SA state hospitals have become, as 58 year old Andre Smit’s family found out when Andre died in hospital on 17 February 2021, after the hospital inexplicably refused him kidney dialysis treatment. Due to Covid the family were barred from helping him themselves and they are convinced he developed kidney failure because of dehydration, from neglect, hunger and thirst in the Tshepong hospital.
Continue reading…
Enjoyed this post? Share it!
#COVIDMANIA, a Politicized Flu, Weaponized by Greedy Powermongers into a Great Reset Which Will Kill More Than Covid19 Itself!
NUMBERS DON’T LIE: Despite all the hype and Covid-19 mania peddled by mainstream media and money grabbing politicians, far more people will, and are still contracting and dying from HIV/AIDS, Cancer, Tuberculosis, Malaria, etc. Shockingly, figures have revealed that lockdown will indeed take more lives than it saves! Truth is the ANC and other globalist liberal governments see Covid-19 as an opportunity not only to line their pockets, but also to hammer through ideological political social engineering projects in the so called Great Reset. For all their claims about saving lives, that really is the last thing on their minds, Socialism is, which is why Covid has been nicknamed #CCPvirus…
Continue reading…
Enjoyed this post? Share it!
12 Day Delay in ANC Government Covid19 Tests! Despite 3 Months Warning & Totalitarian Powers Plus Billions at its Disposal, ANC Totally Failing Fight Against CCP-Virus!
The much vaunted ANC government Covid-19 testing capacity has crashed, as an enormous backlog in CCP-virus tests has developed at the National Health Laboratory Service (NHLS), resulting in a waiting period of between 10-12 days for a test to be concluded, which makes testing pointless, as the genetic material of the virus breaks down after 72 hours! In contrast, private laboratories, which do just over half the CCP-virus tests in the country, just take a day to complete such a test.
Continue reading…
Enjoyed this post? Share it!
National Health Insurance: Medical specialists and doctors threaten to flee overseas
The new National Health Insurance (NHI) that the ANC-regime wants to implement is facing fierce opposition from doctors and medical professionals in the Free State. These medics are currently threatening to go overseas, meanwhile, the Free State DA has also been involved in a fight with Montsent Tsiu, the MEC of Health in the province. The parties involved confirm that the NHI is going to become an unaffordable system that is doomed even before it is implemented.
The doctors support the principle of health care for all but reckon that the NHI is not a feasible system. It is believed that if doctors are first harmed by being prohibited from opening private practices and patients are forced upon them whom they must pay attention within 24 hours, they will simply walk.
According to reports from Network 24, Marietta Pittaway, DA MPW, accused Tsiu of sitting in the Free State Legislature for “prematurely” informing parliament that the Free State provincial government
Continue reading…
Enjoyed this post? Share it!
Misappropriation of R5.8 bil, Afriforum to lay charges – NHI violates constitution
During a media conference held on 18 November 2019, AfriForum launched a comprehensive report on why the implementation of National Health Insurance (NHI) in South Africa will be unconstitutional. The report further explains why the impact study on which the NHI is based, is totally inadequate which means that the Bill should be set aside…
Continue reading…
Enjoyed this post? Share it!
Junk Status looms – Implementation of NHI will have disastrous consequences for SA economy
AfriForum today sent a letter to President Cyril Ramaphosa, Finance Minister Tito Mboweni and Minister of Health Zweli Mkhize warning the civil rights organization that the implementation of national health insurance (NHI) could eventually lead to the downgrading of the country’s credit rating to junk status . This comes after the credit rating agency Moody’s..
Continue reading…
Enjoyed this post? Share it!
LETTER: We were sold out in 1994 – ANC ruined our education system
LETTER – We were sold out in 1994. For 25 years we’ve been ruled by an ANC that could and did shun all other parties as long as it kept its majority and worked within the confines of our Constitution. The ANC has an abusive relationship with the masses who keep it in political power,..
Continue reading…
Enjoyed this post? Share it!
Launching NHI is not going to improve healthcare – SA health services could face a shortfall of 400,000 nurses by 2025
The government’s intention to launch a National Health Insurance already appears to be incoherent. Apart from the only two days the members were given to an advisory committee to determine which medical conditions would be covered, another “massive problem” has now emerged: Prospective nursing staff are hampered by the accreditation of Institutions where they had..
Continue reading…
Enjoyed this post? Share it!
ANC has no plan to fix nursing crisis but still wants NHI
Objections to the ANC’s disastrous National Health Insurance bill close on 11 October! Make sure that you lodge your objection to ensure we Stop The NHI. The Democratic Alliance (DA) can confirm that the ANC government, in its hurried attempt to implement NHI, has no plan to fix the looming nursing crisis in South Africa..
Continue reading…
Enjoyed this post? Share it!
Your new life under South Africa’s new NHI according to economist Dawie Roodt
This is an opinion piece by Dawie Roodt, chief economist of the Efficient Group. It’s the year 2026 and we are all celebrating; the National Health Insurance (NHI) has just been implemented. Everyone in South Africa is now entitled to free, world-class health services. It certainly wasn’t easy, but finally, the dream is a reality!..
Continue reading…
Enjoyed this post? Share it!
ANC regime’s NHI plan back in the news – according to spokesman it will be wisely implemented – As if the ANC knows what wisely means!
The ANC’s National Health Plan is back in the news after the party’s spokesman said the scheme would be implemented with “prudence”.
Continue reading…
Enjoyed this post? Share it!
National Health Insurance Plan of ANC regime – this is what you need to know!
The government is going to stop private medical aids! The government is going to force people to become part of the state’s National Health Insurance (NHI) Fund – people have no choice. This means an ANC official is now going to decide who your doctor is and what hospital families can go to, even if..
Continue reading…
Enjoyed this post? Share it!
Health care shares dropped R14 billion since announcement of NHI
The FF Plus is seriously worried about the negative impact that the tabling of the National Health Insurance (NHI) Bill in Parliament last Thursday has since had on the country’s economy. It is not only the Discovery group’s shares that fell on the Johannesburg Stock Exchange. Yesterday, an amount of R14 billion was lost in..
Continue reading…
Enjoyed this post? Share it!
Registered illegal aliens from other countries will have access to all medical services under the NHI, which will be financed by South Africa’s hard-working taxpayers
The government’s plan to steamroller the National Health Insurance (NHI) through Parliament and to have it promulgated as legislation will cost South Africa dearly. Last month, the FF Plus warned in Parliament that adopting the NHI as legislation and enforcing it will cause experienced medical professionals to leave the country. The Minister of Health, Dr..
Continue reading…
Enjoyed this post? Share it!
Dating SA
Submit Stories
Internet Florist
Instant Loans
Qatar Airways
Recent Posts:
- Expressing support for the Boer cause in the unholy hellscape of South Africa has serious consequences. February 14, 2024
- (no title) October 1, 2023
- Why Should Building Project Owners Hire Architecture Firms? November 18, 2022
- Giorgia Meloni, “Italy’s Trump”, Favoured To Become First Female PM in Coalition with Salvini & Berlusconi September 23, 2022
- Studies Show Online Dating has Shaken off the Old Stigma and is Fully Mainstream Now! August 30, 2022
- VIDEO: PROOF MSM & Big Tech Stole US Election With Censorship! 17% Biden Voters REGRET Vote – Would NOT Have Voted Biden Had They Known About Biden Scandals! August 30, 2022
- The Best Indoor Home Security Cameras for 2022 August 19, 2022
- Are Globalists Planning to Charge us to Breathe? What is your breath worth? August 14, 2022
- SA Farmers Next? Ireland also Attacks their Farmers, Like the Netherlands, Germany and Canada! August 4, 2022
- SAAI Discloses Land Claims Database Online! Files Contempt of Court Against Agriculture Minister Thoko Didiza July 29, 2022
- Globalist Campaign Painting Farmers as “The Enemy of The State”, Strikes The Netherlands & Belgium July 17, 2022
- Petition: Make Peace NOT War! Invite both Ukraine & Russia to join NATO & EU to ensure lasting peace! February 27, 2022
- Young South African Jailed for Life in Thailand after Signing for Parcel Containing Drugs, Addressed to her Employer! February 19, 2022
- #InterNazi – Will Hitlerisation of Putin backfire and expose the InterNational Socialist’s deceit and treachery in WWI & II? February 14, 2022
- Send Valentine’s Flowers & Gifts to Your Loved One Online Today! February 7, 2022
- IMF & World Banksters used ANC & “anti-racism” to Trick South Africa into Permanent Debt Slavery! December 11, 2021
- #HolodomorDenial: the Genocide of 7 Million Ukrainians, Many of them Christians, That Jews Deny… November 28, 2021
- Has Corporate SA Been Infected by ANC Corruption, Greed & Negligence? Dimension Data NTT Case Study October 27, 2021
- Racist NPA! Black Taxi Driver who Killed White Father & Son NOT Charged yet Whites are Charged Without Bail for far Less! October 21, 2021
- FF+ Election Manifesto Calls for Scrapping of BBBEE – PaNazi Lesufi Replies that BEE will stay “until the sins of white ancestors are wiped out”! October 18, 2021
Search SA News
News Headlines
Links
- C.V.co.za
- Yell.co.za Free Ads
- BokWeb Hosting
- SpeedDating.co.za
- The Cape
- SAFFA.com
- Dating South Africa
- SA-Radio.com
- MedSure
- Health
Topics:

Buy Groceries Online for Delivery!
Cheap Travel Deals
Subscribe for Free South Africa News
Search SA News Headlines
Yell Dating Online
Samsung Phone From R99
Teach English
Come Chat Online!

Accommodation Deals
 Yell.co.za New Listings
Yell.co.za New Listings
Kaspersky Antivirus
Gratis Aanlyn Winkels!

Cheap Flights @Sky.co.za
Find a Hotel:
Hand Delivered Flowers
Share and Follow SA-News on Social Media:
Follow @SAnewscom on Twitter
 SAFFA.com News
SAFFA.com News
- Sickness Doesn’t Take a Vacation: 7 Steps to Managing Illness While Travelling
- Prankster Tricks London Gatwick Airport Passengers into Thinking They Were Landing at London Luton Airport!
- SAAI Discloses Land Claims Database Online! Files Contempt of Court Against Agriculture Minister Thoko Didiza
- Globalist Campaign Painting Farmers as “The Enemy of The State”, Strikes The Netherlands & Belgium
- Petition: Make Peace NOT War! Invite both Ukraine & Russia to join NATO & EU to ensure lasting peace!